Nov29, 2023
DOA - 27/11/2023
CHIEF COMPLAINTS:
Fever since 1 week
Palpitations since 1 week
Generalised weakness since 4 days
Blood in stools since 3 days
Chest pain and tightness since 4 days
HISTORY OF PRESENTING ILLNESS
The patient was apparently asymptomatic 1 week ago and then she developed fever which is sudden in onset, high grade, associated with chills and rigors, relieved temporarily on medication.
Palpitations are present since 1 week which are regular and associated with chest discomfort
There is h/o shortness of breath on exertion which is progressive (grade 2 to grade 3). No orthopnea, or PND.
There is associated generalised weakness since 4 days and blood in stools since 3 days.
There is no h/o vomitings, loose stools, pain abdomen, giddiness.
PAST HISTORY
N/k/c/o DM, HTN, Asthma, TB, Epilepsy, CAD, CVA
There is h/o tubectomy
PERSONAL HISTORY
Diet mixed
Appetite normal
Sleep adequate
Bowel movement- Constipation present, Bladder regular
Addictions - None
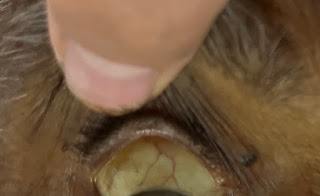
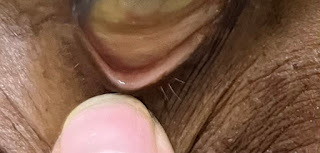
GENERAL EXAMINATION
SYSTEMIC EXAMINATION
INVESTIGATIONS
PROVISIONAL DIAGNOSIS
Megaloblastic Anemia
TREATMENT
27/11/23-
1 unit PRBC Transfusion
Inj Pan 40mg IV OD
Inj Iron sucrose 200mg in 100ml NS IV OD
Inj Vitcofol 1500mg in 100ml NS IV OD
Strict I/O charting, monitor vitals, inform sos
28/11/23-
1 unit PRBC transfusion
Inj Ceftriaxone 2g IV BD
Cap Doxycycline 100mg PO BD
Inj Pan 40mg IV OD
Inj Iron sucrose 200mg in 100ml NS IV OD
Inj Vitcofol 1500mg in 100ml NS IV OD
Strict I/O charting, monitor vitals, inform sos









Comments
Post a Comment